UPDATE! 09.06.2016: UN-CRC reprimanded Nepal for IGM and Bullying!
 “All children underwent tubularized incised plate urethroplasty”
“All children underwent tubularized incised plate urethroplasty”
![]() This week, at the 72nd Session of the UN Committee on the Rights of the Child (CRC), Nepal is first up for review of Intersex Human Rights including the “growing practice of Intersex Genital Mutilations” on Thur 19 May 15:00-18:00h CET [Nepal: 18:45-21:45h] + Fri 20 May 10:00-13:00h CET [Nepal: 12:45-16:45h] – archived on treatybodywebcast.org!
This week, at the 72nd Session of the UN Committee on the Rights of the Child (CRC), Nepal is first up for review of Intersex Human Rights including the “growing practice of Intersex Genital Mutilations” on Thur 19 May 15:00-18:00h CET [Nepal: 18:45-21:45h] + Fri 20 May 10:00-13:00h CET [Nepal: 12:45-16:45h] – archived on treatybodywebcast.org!
Next week: The UK …
TABLE OF CONTENTS “Intersex Genital Mutilations, Stigma and Bullying in Nepal”
1. Background: 1st Intersex Workshop, Intersex Stories Book, 2016 CRC NGO Report
2. Intersex Genital Mutilations in Nepali Paediatric Hospitals
a) IGM in Publications by Doctors and Hospitals
b) IGM in Witnesses Accounts
3. Denial of Needed Health Care
4. Stigma, Bullying and Isolation
• Nepal questioned over IGM by UN Child Rights Committee – Gov denies
2. Intersex Genital Mutilations in Nepali Paediatric Hospitals
SUMMARY: Despite that the 1st Intersex National Workshop identified “Intersex genital mutilation as a growing practice in Nepal” and recommended to “Prohibit medically unnecessary surgery and procedures without informed consent”, seconded by the 2016 NGO Report to CRC, no research or documentation on IGM practices in Nepal could be found.
While far from exhaustive, this section thus collects evidence, so far substantiating
- IGM1 “Masculinising Genital Corrections” incl. “Hypospadias Repair” regular practiced in at least 2 Nepali children’s clinics in Kathmandu and Basundhara, as well possibly also in non-paediatric clinics in other regions
- the recently achieved capability for laparoscopic gonadectomies a.k.a IGM3 Sterilising Procedures in at least 1 children’s clinic in Kathmandu
- doctors and clinics openly advertising IGM1 as beneficient and safe, and aiming to expand the practice within the (positive) overall drive to allow more children access to (necessary) paediatric treatments
Witness accounts from Nepal further link IGM1 to 2 additional Government and University Children’s Clinics in Kathmandu and Dhulikel.
a) IGM in Publications by Nepali Doctors and Hospitals
Kanti Children’s Hospital (Kathmandu):
• IGM 1 “Hypospadias Repair”
• Capability for IGM3 Sterilising Procedures (“Laporoscopic Gonadectomy”).
Source: Hospital Homepage, http://kantichildrenhospital.gov.np/paedratic-surgery/
“We have started performing Snodgra[ss] TIP Urethroplasty for proximal penile hypospadias“
“We feel proud to mention that we have started dedicated pediatric laparoscopic surgical services this year.”
“Facilities available at surgical unit:
[…]
Pediatric Laparoscopic Surgery.
Pediatric Urology. […]”
Kanti Government Children’s Hospital (Kathmandu) and BP Smriti Hospital (Basundhara):
• IGM 1 “Hypospadias Repair” practiced regularly
Source: Journal of Nepal Paediatric Society, J Nepal Paediatr Soc 2014;34(1):29-33, http://www.nepjol.info/index.php/JNPS/article/view/8692
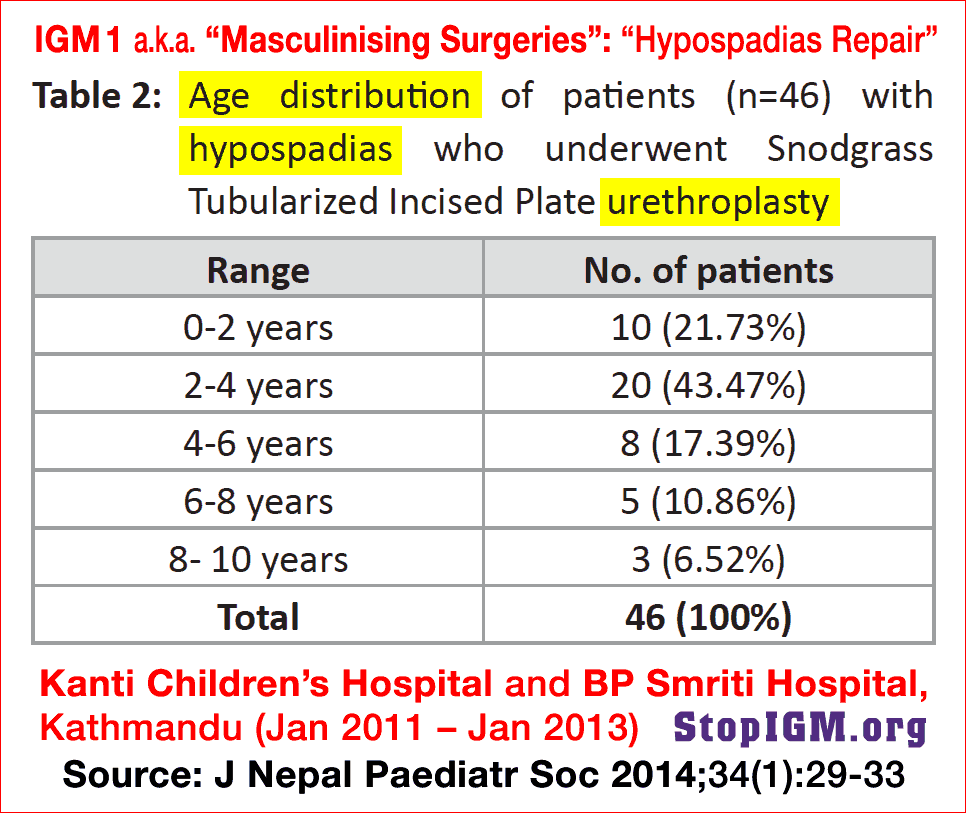
“A total of 46 male children 18 months to 10 years age with penile hypospadias were included in this study from January 2011 to January 2013 in Kanti Children’s Hospital and BP Smriti Hospital. Only distal and mid penile hypospadias with good and wide urethral plate were included. All children underwent tubularized incised plate urethroplasty described by Snodgrass. Hypospadias with moderate to severe chordee were excluded.”

“Each patient was assessed on the 8th-10th postoperative day after removal of the catheter and during their first follow-up on two weeks after discharge. Assessment was done on the basis complications like urethrocutaneous fistula, meatal stenosis, cosmetic look of penis and glans and urinary stream.”
“The overall complication rate requiring surgical intervention was 8 (17.3%). Mean duration of surgery was 66 minutes (60-80 minutes). Urethrocutaneous fistula occurred in 5 (10.8%), meatal stenosis in 1 (2.1%) and wound dehiscence in 2 (4.3%) patient.”
“Tubularized incised plate urethroplasty is a simple, single stage surgery for distal hypospadias. It gives good functional neourethra of normal looking glans and meatus with a low rate of complications like urethrocutaneous fistula, stricture. It is our preferred method of repairing distal and midpenile hypospadias in our institution.”
N O T E : This articles gives NO INDICATION at all of any mean follow-up time! Arguably follow-time was in maximum the 24 months of the study – with severe and dangerous complications, particularly urethral strictures and stenoses, drastically increasing only later in life …
B.P. Koirala Institute of Health Sciences (Dharan)
• IGM 1 “Hypospadias Repair” practiced regularly
[on persons of unkown age, see N O T E below]
Source: Plastic Surgery International, Volume 2011 (2011), Article ID 870902, http://www.hindawi.com/journals/psi/2011/870902/
“B.P. Koirala Institute of Health Sciences, Dharan, Nepal, is the only tertiary care referral centre in the eastern region of Nepal. This paper discusses the author’s experience of starting a plastic surgery unit in eastern Nepal regarding need and present status of plastic surgery care in Nepal. Methods. We analyzed the data of patients treated in Plastic surgery unit from July 2007 to February 2009. We did evaluation regarding type of patients, procedures, and their outcome.”
“Other congenital anomalies included clefts [1] and hypospadias [2] hands and foot anomalies (Figure 4).”
Table 4: Details of various plastic surgery procedures.
––––––––––––––––––––––––––––––––––––––––––––
Cleft n = 7
––––––––––––––––––––––––––––––––––––––––––––
Cleft lip repair 4
Palatoplasty 1
cleft lip nose rhinoplasty 2
––––––––––––––––––––––––––––––––––––––––––––
[…]
––––––––––––––––––––––––––––––––––––––––––––
Genitourinary reconstructions n = 1 2
––––––––––––––––––––––––––––––––––––––––––––
Hypospadias repair 8
Penile fracture 1
Filarial scrotum and penis 3
––––––––––––––––––––––––––––––––––––––––––––
[…]
––––––––––––––––––––––––––––––––––––––––––––
Hand and upper extremity reconstruction n = 3 9
––––––––––––––––––––––––––––––––––––––––––––
[…]
Polydactyly 1
[…]
––––––––––––––––––––––––––––––––––––––––––––
[…]”“Our observation shows that the role of plastic surgeon becomes more vital in centres where other specialty services are lacking, as plastic surgeons can handle variety of situations because of their training [2]:
[…]
(vi) quality management of hypospadias/epispadias patients in absence of urosurgeons/paediatric surgeons,
[…]There is increasing demand for plastic surgery services because of growing public awareness for complete cure, reduction of morbidity, and limitation of deformity which indirectly helps in productivity of population. […]”
N O T E : The article doesn’t contain any reference to actual outcomes of the “Hypospadias repair,” nor to the age of the “patients”. The grouping together with “clefts [1] and […] hands and foot anomalies (Figure 4)” however may indicate an increased probability of involuntary treatments on children.
b) IGM in Witnesses Accounts
Esan Regmi and Parsu Ram Rai, the authors of the Thematic Intersex NGO Report to CRC, reported during a skype interview on 16.05.2015 that, while visiting the hospitals in question as patients, witnesses personally known to them recently learned of further cases of IGM1 “Masculinising Surgeries” in the following clinics:
- Dhulikhel Hospital, Kathmandu University Hospital (Dulikel):
3 children (aged 20 months, 5 years, and 7 years)
- National Academy of Medical Sciences, Bir Hospital (Kathmandu):
1 child (aged 13 years)
TABLE OF CONTENTS “Intersex Genital Mutilations, Stigma and Bullying in Nepal”
1. Background: 1st Intersex Workshop, Intersex Stories Book, 2016 CRC NGO Report
2. Intersex Genital Mutilations in Nepali Paediatric Hospitals
a) IGM in Publications by Doctors and Hospitals
b) IGM in Witnesses Accounts
3. Denial of Needed Health Care
4. Stigma, Bullying and Isolation
• Nepal questioned over IGM by UN Child Rights Committee – Gov denies
See also:
• 11 Verdicts by UN Treaty Bodies Condemning IGM – And Counting …
• UN Committee for the Rights of the Child (CRC) 2015: IGM = Harmful Practice
• UN Committee against Torture (CAT) 2015: IGM = Inhuman Treatment or Torture
• UN Human Rights Committee (HRCttee) to examine IGM Practices
• UN Committee on the Rights of Persons with Disabilities (CRPD) condems IGM
• Historic 56th Session of Committee against Torture reprimands 4 Governments over IGM
• CAT 2011: Germany must investigate IGM practices and compensate survivors!
Intersex Genital Mutilations • 17 Most Common Forms
Human Rights Violations Of Children With Variations Of Sex Anatomy
IGM – Historical Overview • What is Intersex? • How Common are IGMs?
>>> Download PDF (3.65 MB) >>> Table of Contents
Eliminating IGM practices by holding the perpetrators accountable via well-established applicable human rights frameworks, including Inhuman Treatment and Harmful Practices – Presentation @ UN expert meeting on Intersex Human Rights in Geneva 26.–27.10.2015
>>> Download PDF (831kb)


